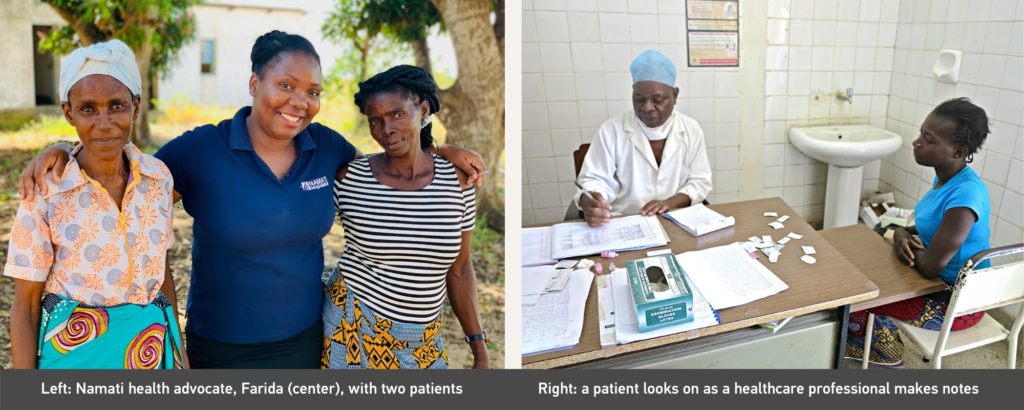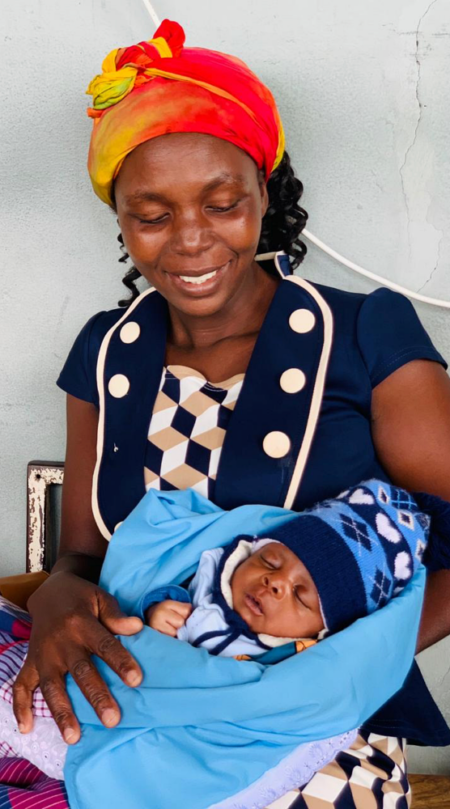
A woman and her newborn await their postnatal visit at Nhongonhane Health Center in Marracuene District
Our Journey in 2019 & 2020
Our failure to deliver decent healthcare to all people is not just a technocratic problem, relating to the way we resource and design the delivery of services. It’s also a justice problem, stemming from imbalances of power between people and the healthcare system, and between frontline staff and the institutions that employ them.
When people don’t understand and exercise their rights, they are vulnerable to abusive and disrespectful care: exam rooms that offer no privacy, health facilities without a functioning toilet, or health workers who demand a bribe for treatment. When these experiences accumulate, people lose faith in the health system and many opt to stay away, forgoing critical care like postpartum services and HIV treatment.
Our Grassroots Impact at a Glance
In 2019 and 2020, paralegals supported thousands of people to resolve breakdowns in healthcare delivery. Together, they improved life saving services for entire communities.



Maria was made to pay for a blood transfusion she received after hemorrhaging during labor.
Paying for Blood: Bribery in Mozambique’s Healthcare System
The labor pains came as no surprise. Maria* was nine months pregnant with her second child; she knew what to expect. But as she made her way to the local health center where she was to give birth, Maria began to bleed. By the time she arrived, she was hemorrhaging.
The nurse on duty quickly arranged for an ambulance to take her to Quissico District Hospital for a blood transfusion. Fortunately, Maria survived. Her baby, however, did not.
Later that night, as Maria was preparing to be discharged, a nurse approached and told her that she had to pay the equivalent of 70 USD for the blood and plasma she had received. It was a huge sum for Maria, who, like many Mozambicans, gets by on the food she farms and the small amount she makes selling some of her harvest at the market.
“I was outraged,” recalls Maria. “[But the nurse] said there’s no other way. ‘You can’t leave here until you pay. That’s the law.”